Scalp eczema is a common skin condition that causes red, itchy, and scaly patches on the scalp. If you’re dealing with flaking, irritation, or discomfort on your scalp, you’re not alone—this chronic condition affects millions of people. The good news? Effective treatment options are available to help you manage symptoms and prevent flare-ups.
TLDR: Key Takeaways
- Scalp eczema is treatable: Medicated shampoos with ingredients like ketoconazole, zinc pyrithione, and salicylic acid effectively manage symptoms
- Multiple types exist: Seborrheic dermatitis is the most common type, affecting the scalp, while atopic dermatitis and contact dermatitis can also occur
- Gentle care matters: Use mild baby shampoo, avoid harsh chemicals in hair products, and wash with warm water to protect your skin barrier
- Seek professional help when needed: If over-the-counter treatments don’t work within 2-3 weeks, or if you experience significant hair loss or mental health impacts, consult a healthcare provider
Get Fast, Affordable Treatment for Scalp Eczema
Living with scalp eczema doesn’t have to mean endless waiting rooms and expensive dermatologist visits. At MyInstantMD, our licensed providers can evaluate your symptoms, recommend the right treatment options, and prescribe medicated shampoos or other medications you need—all from the comfort of your home.
For just $59.99, you can receive a personalized treatment plan within minutes. No appointments, no hassle, just quality care when you need it. Get treatment for eczema online and start feeling relief today.
Understanding Scalp Eczema
Scalp eczema is an umbrella term for inflammatory skin conditions affecting the scalp. The most common type of eczema that affects the scalp is seborrheic dermatitis (also spelled seborrhoeic dermatitis), which causes scaly skin, redness, and persistent itching. According to the American Academy of Dermatology, seborrheic dermatitis typically develops in oily areas of the body, including the scalp, face, and chest.
Another type that can affect the scalp is atopic dermatitis (also called atopic eczema), which is often linked to a weakened skin barrier and immune system responses. The National Eczema Association notes that understanding which type of eczema you have is essential for choosing the right treatment approach.
What Causes Scalp Eczema?
The exact cause of scalp eczema isn’t fully understood, but several factors contribute to scalp eczema flares:
- Malassezia yeast: This naturally occurring fungus on the skin can trigger inflammation
- Hormonal changes: Fluctuations can make eczema worse
- Immune system dysfunction: An overactive immune response to normal stimuli
- Allergic reaction: Sensitivity to hair products or styling products containing harsh chemicals
- Environmental triggers: Stress, cold weather, and dry conditions
Contact dermatitis, another skin condition, can also affect the scalp when you have an allergic reaction to ingredients in hair spray, perm solutions, or other hair products.
How to Treat Scalp Eczema: Effective Treatment Options
Medicated Shampoos
Medicated shampoos are the first-line treatment for scalp eczema. These specialized products contain active ingredients that target inflammation, reduce fungal infection, and help restore the skin’s protective layer.
Key ingredients to look for:
- Ketoconazole shampoo: An antifungal ingredient that combats Malassezia yeast
- Zinc pyrithione: Reduces fungal growth and has antibacterial properties
- Salicylic acid: Helps remove scaly patches and dead skin cells from the hair shaft
- Coal tar: Slows down excessive skin cell production
Mayo Clinic recommends alternating between different medicated shampoos if one stops working effectively. Both over-the-counter shampoos and prescription shampoo options can be effective, depending on the severity of your condition.

Gentle Hair Care Practices
Proper hair care is crucial when managing scalp eczema:
- Use a mild baby shampoo on non-treatment days to avoid shampoos with harsh chemicals
- Wash your hair with warm water instead of hot water, which can dry out affected areas
- Apply products to keep your hair slightly greasy, as moisture helps the skin barrier
- Limit heat styling—use hair dryers on a cool setting to prevent further irritation
- Perform a patch test before trying new hair products to check for allergic reactions
Topical Products and Natural Remedies
Beyond medicated shampoos, several topical products can provide relief:
- Mineral oil or olive oil: Apply to patches of skin, cover with a shower cap for 30 minutes, then wash out to soften scales
- Tea tree oil: Has natural antifungal properties (dilute before applying)
- Prescription topical corticosteroids for severe eczema flare episodes
- Moisturizers that strengthen the protective layer of the scalp
If you’re struggling with other forms of eczema on your body, you can learn more about eczema and explore online treatment for skin rashes to address multiple concerns at once.
When to See a Healthcare Provider
Consult a healthcare provider if:
- Over-the-counter treatments don’t improve symptoms after 2-3 weeks
- You experience significant hair loss from affected areas
- The condition impacts your mental health or daily activities
- You notice signs of a secondary fungal infection or worsening symptoms
- You’re unsure whether you have scalp eczema, dandruff, psoriasis, or another condition
Seborrheic dermatitis shares symptoms with other papulosquamous diseases like psoriasis, making professional diagnosis important. Clinical considerations and medical sciences have shown that proper identification leads to better treatment outcomes.
Special Considerations
Cradle Cap in Infants
When scalp eczema affects a baby’s scalp, it’s often called cradle cap. This mild form typically resolves on its own, but gentle treatment can help. Use a mild baby shampoo and carefully brush away flakes after applying mineral oil or olive oil to soften them.
Triggers to Avoid
Preventing flare-ups means identifying and avoiding triggers:
- Hair products with harsh chemicals or strong fragrances
- Styling products that contain alcohol or sulfates
- Perm solutions and chemical treatments
- Excessive use of hair spray
- Prolonged exposure to cold, dry weather
Lifestyle Factors
Managing scalp eczema as a chronic condition requires attention to lifestyle factors. Stress, poor sleep, and hormonal changes can all trigger eczema flare episodes. Taking a holistic approach that includes stress management supports your skin’s natural healing process.
If you’re dealing with scalp conditions that might be confused with eczema, such as scalp acne, you might benefit from scalp acne treatment or learning about various types of skin rashes to better understand your symptoms.
Getting Professional Help for Scalp Eczema
While many cases of scalp eczema respond well to over-the-counter options, persistent or severe cases benefit from professional medical evaluation. A healthcare provider can prescribe stronger treatments, help identify triggers, and create a personalized management plan.
Learn more about atopic dermatitis from the AAD to understand how this type of eczema differs from seborrheic dermatitis and what specific treatments work best.
If you need convenient access to treatment without the hassle of scheduling in-person appointments, consider getting treatment for eczema online where licensed providers can evaluate your symptoms and prescribe appropriate medications.
According to the National Institute of Arthritis and Musculoskeletal and Skin Diseases, early intervention and consistent treatment are key to managing eczema long-term and preventing complications.
Frequently Asked Questions About Scalp Eczema
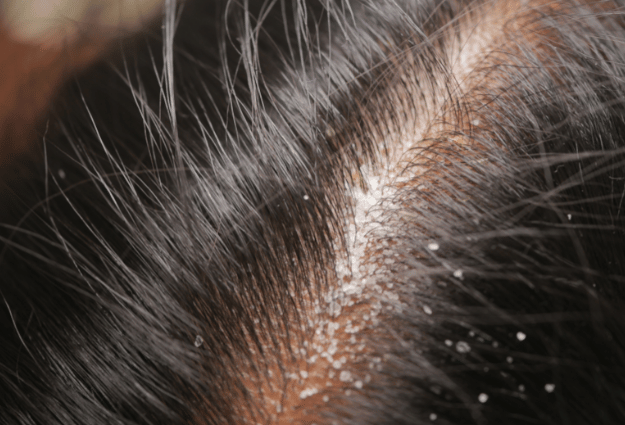
What’s the difference between scalp eczema and dandruff?
While both cause flaking, scalp eczema involves inflammation and produces thicker, more adherent scaly skin compared to the fine, loose flakes of simple dandruff. Seborrheic dermatitis is actually a severe form of dandruff that causes more pronounced redness and irritation on the scalp and other oily areas of the body.
Can hair products make my eczema worse?
Yes, certain hair products containing harsh chemicals can trigger contact dermatitis or make existing eczema worse. Ingredients in styling products, hair spray, and perm solutions may cause an allergic reaction that damages the skin barrier. Always perform a patch test with new products and avoid shampoos that contain sulfates, parabens, or artificial fragrances.
Will scalp eczema cause permanent hair loss?
Hair loss from scalp eczema is usually temporary. When inflammation affects the hair shaft and follicles in affected areas, it can lead to shedding. However, once the eczema flare is controlled and the skin heals, hair typically grows back. Consistent treatment helps prevent flare-ups and protects against long-term damage.
How does seborrheic dermatitis differ from other papulosquamous diseases like psoriasis?
Seborrheic dermatitis and psoriasis are both papulosquamous diseases, but they have distinct characteristics. Seborrheic dermatitis typically affects oily areas and produces yellowish, greasy scales, while psoriasis creates thicker, silvery scales. Other papulosquamous diseases may require different clinical considerations and treatment approaches based on how they affect skin cells and the immune system.
Can I treat my baby’s scalp eczema (cradle cap) at home?
Mild cradle cap on a baby’s scalp can often be managed at home using a mild baby shampoo and gentle brushing. Apply mineral oil or olive oil to soften the scales, wait 30 minutes (you can use a shower cap to prevent mess), then gently wash with warm water. Avoid harsh chemicals and never pick at the scales, as this can damage your baby’s delicate skin barrier.
How long does it take for scalp eczema treatment to work?
Most people see improvement within 2-4 weeks of starting treatment with medicated shampoos or topical products. Over-the-counter options containing an active ingredient like zinc pyrithione, salicylic acid, or ketoconazole shampoo typically show results within this timeframe. If you don’t see improvement or your symptoms get worse, consult a healthcare provider who may recommend prescription shampoo or other treatment options for this chronic condition.




