Eczema, or atopic dermatitis, is a chronic skin condition affecting millions of people worldwide. Finding the best treatment for eczema often requires a personalized approach based on symptom severity, affected areas, and individual triggers. While there’s no permanent cure, effective management strategies can significantly improve symptoms and quality of life.
TLDR: Key Points About Eczema Treatment
- Daily moisturizing with ceramide-rich products forms the foundation of eczema management
- Topical corticosteroids are effective for controlling inflammation during flares
- Non-steroidal options like calcineurin inhibitors work well for sensitive areas and long-term use
- Advanced treatments including biologics, oral medications, and phototherapy are available for moderate-to-severe cases
- Identifying and avoiding personal triggers is crucial for preventing flares
Ready to Get Relief from Eczema?
If you’re struggling with eczema symptoms and need expert guidance for a personalized treatment plan, MyInstantMD can help. Our board-certified providers can evaluate your eczema, recommend appropriate treatments, and prescribe medications if needed—all from the comfort of your home.
No waiting rooms, no appointment scheduling hassles, and treatment plans tailored to your specific needs. Get started with convenient online eczema treatment today for just $59.99.
Understanding Eczema and Its Symptoms
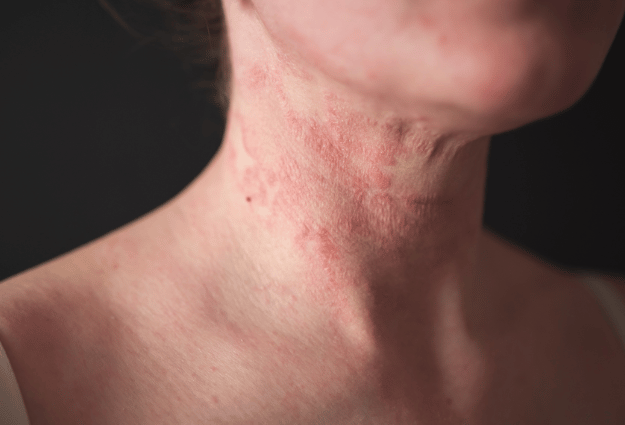
Eczema is characterized by red, itchy, and inflamed skin that can appear anywhere on the body. The condition occurs when your skin barrier function is compromised, leading to moisture loss and increased vulnerability to irritants and allergens.
Common eczema symptoms include:
- Dry, scaly skin
- Intense itching (particularly at night)
- Red, inflamed patches
- Rough or leathery skin texture
- Small, raised bumps that may leak fluid
- Sensitive skin that reacts easily to irritants
First-Line Treatments for Eczema
Moisturizing and Barrier Repair
Consistent moisturizing forms the foundation of eczema treatment. According to research published by the National Center for Biotechnology Information, maintaining skin hydration is crucial for managing symptoms and preventing flare ups.
Best practices for moisturizing:
- Apply moisturizer within 3 minutes after bathing to lock in moisture
- Choose fragrance-free, thick creams or ointments rather than lotions
- Use products containing ceramides to help repair the skin barrier
- Apply moisturizers at least twice daily, or more frequently on dry skin areas
Topical Steroids for Inflammation Control
Topical corticosteroids remain the gold standard for controlling eczema flares. The American Academy of Dermatology recommends these medications as first-line treatment for reducing inflammation and itching during active flares.
Different strengths are available:
- Mild (like hydrocortisone 1%) for face, genitals, and skin folds
- Moderate to potent options for body areas during significant flares
- Super-potent formulations for severe, localized patches (short-term use only)
When used correctly under medical guidance, topical steroids are safe and effective for most patients. However, they should be used as directed to avoid potential side effects from prolonged use.
Non-Steroidal Topical Medications
For patients concerned about steroid use or for sensitive areas, non-steroidal options include:
Topical calcineurin inhibitors (tacrolimus, pimecrolimus): These medications block certain immune system pathways that trigger inflammation without the skin-thinning effects of steroids, making them suitable for long-term use on delicate areas like the face and neck.
Phosphodiesterase-4 inhibitors (crisaborole): This newer class of medication reduces inflammation and can be used for mild to moderate eczema in patients 2 years and older.
Advanced Treatments for Moderate to Severe Eczema

When topical treatments aren’t providing adequate relief, healthcare providers may recommend more advanced options.
Systemic Medications
For severe or widespread eczema, oral or injectable medications that work throughout the body may be necessary:
Biologics: These targeted treatments block specific pathways in the immune system that contribute to inflammation. Dupilumab was the first biologic approved for moderate to severe atopic dermatitis and works by blocking key inflammatory signals (IL-4 and IL-13).
Oral immunosuppressants: Medications like cyclosporine, methotrexate, or azathioprine may be used for short periods in severe cases. These require careful monitoring due to potential side effects.
JAK inhibitors: Newer oral medications like upadacitinib and abrocitinib target specific enzymes involved in inflammation and have shown promising results for moderate to severe eczema.
Light Therapy (Phototherapy)
Light therapy uses controlled exposure to specific wavelengths of ultraviolet light to reduce inflammation and itch. According to the National Eczema Association, narrowband UVB phototherapy can be particularly effective for widespread eczema that doesn’t respond adequately to topical treatments.
Benefits include:
- Non-pharmaceutical option
- Effective for widespread disease
- Can be combined with other treatments
- Potentially induces longer remission periods
However, it requires regular sessions at a medical facility and may not be suitable for all patients.
Specialized Approaches for Difficult Cases
Wet Wrap Therapy
For intense flares or particularly stubborn areas, wet wrap therapy can provide significant relief. This technique involves:
- Applying medication and moisturizer to affected areas
- Wrapping the area with a wet layer of gauze or cloth
- Covering with a dry outer layer
- Leaving in place for several hours or overnight
This method enhances medication absorption while soothing inflamed skin and preventing scratching.
Managing Environmental Triggers
Identifying and avoiding triggers is essential for preventing eczema flares. Common triggers include:
- Harsh soaps and detergents
- Certain fabrics (especially wool and synthetic materials)
- Extreme temperatures and sweating
- Allergens like dust mites, pet dander, or pollen
- Stress and hormonal changes
Using gentle cleansers, wearing cotton clothing, maintaining moderate home temperature and humidity, and practicing stress reduction can all help reduce flare frequency.
Creating a Comprehensive Treatment Plan
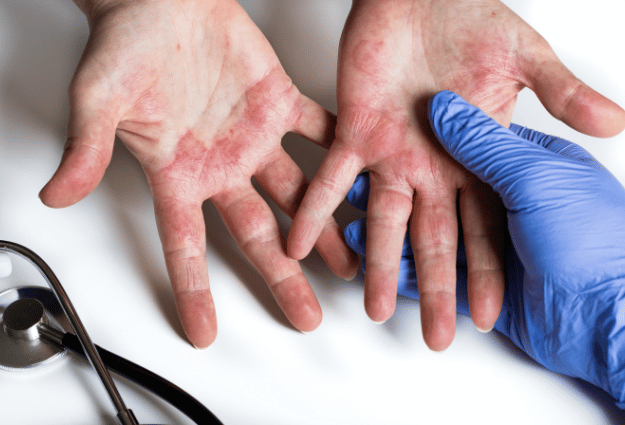
The best treatment for eczema usually involves a personalized, multi-faceted approach. Working with a healthcare provider to develop a treatment plan is important, especially for moderate to severe cases.
A complete plan typically includes:
- Daily skin care routine with appropriate cleansers and moisturizers
- Medications for managing acute flares
- Maintenance therapy to prevent future flares
- Identification and avoidance of personal triggers
- Strategies for managing itch and sleep disruption
- Regular follow-up with healthcare providers to adjust treatment as needed
FAQ: Common Questions About Eczema Treatment
How can I manage eczema symptoms at home?
Home management starts with gentle skin care and trigger avoidance. Use lukewarm (not hot) water for bathing, pat skin dry instead of rubbing, apply moisturizer immediately after bathing, wear loose cotton clothing, and keep fingernails short to minimize damage from scratching. Natural oils like coconut oil or sunflower seed oil may provide additional moisture for some people.
Can food allergies make my eczema worse?
Food allergies can trigger eczema flares in some individuals, particularly children. Common food triggers include dairy, eggs, nuts, soy, gluten, and certain fruits. If you suspect certain foods worsen your symptoms, consult with an allergist for proper testing rather than eliminating multiple foods without guidance.
Is seborrheic dermatitis different from regular eczema?
Yes, seborrheic dermatitis is a distinct type of eczema that primarily affects the scalp and face, particularly in areas with many oil glands. It creates reddish, greasy-looking scales and can be triggered by a yeast called Malassezia that normally lives on the skin. Treatment typically includes antifungal shampoos or creams rather than traditional eczema therapies.
How can I reduce itching from eczema?
To reduce itching, keep fingernails short, apply cold compresses to itchy areas, use anti-itch moisturizers containing colloidal oatmeal or 1% hydrocortisone, take oral antihistamines (especially at night), and consider an oatmeal bath for widespread itching. Avoid scratching, which can lead to the “itch-scratch cycle” and skin infections.
Can contact dermatitis be related to my eczema?
Contact dermatitis is a form of skin rash that occurs when skin comes into direct contact with an irritant or allergen. While it’s technically different from atopic dermatitis, people with atopic eczema often have more sensitive skin and may be more prone to developing contact dermatitis from substances like metals (especially nickel), fragrances, preservatives, or latex.
What treatments work for pediatric patients with eczema?
Children with eczema require gentle approaches. Treatment typically includes regular moisturizing, mild topical corticosteroids, trigger avoidance, and special attention to your child’s skin during bathing. For moderate to severe cases, topical calcineurin inhibitors, phototherapy, or even biologics may be considered under close medical supervision. Wet wrap therapy can be particularly effective for severe flares in children.




